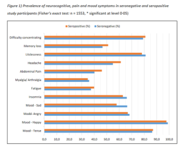
Folgeerscheinungen bei Erwachsenen 6 Monate nach der COVID-19-Infektion
Jennifer K. Logue, BS1;
Nicholas M. Franko, BS1;
Denise J. McCulloch, MD, MPH1; et al
Dylan McDonald, BA1;
Ariana Magedson, BS1;
Caitlin R. Wolf, BS1;
Helen Y. Chu, MD, MPH1
Autorenverbindungen
Artikelinformationen
JAMA-Netz geöffnet. 2021;4(2):e210830. doi:10.1001/jamanetworkopen.2021.0830
COVID-19-Ressourcenze
Einführung
Viele Menschen erleben anhaltende Symptome und eine Verschlechterung der gesundheitsbezogenen Lebensqualität (HRQoL) nach der Erkrankung der Coronavirus-Krankheit 2019 (COVID-19).
1 Vorhandene Studien konzentrierten sich auf hospitalisierte Personen 30 bis 90 Tage nach Krankheitsbeginn
2 –
4 und berichteten über Symptome bis zu 110 Tage nach der Krankheit.
3 Langzeitfolgen bei ambulanten Patienten sind nicht gut charakterisiert.
Methoden
Eine prospektive Langzeitkohorte von Erwachsenen mit laborbestätigter Infektion mit dem schweren akuten respiratorischen Syndrom Coronavirus 2 (SARS-CoV-2) wurde an der University of Washington mit einer gleichzeitigen Kohorte
gesunder Patienten in einer Kontrollgruppe (eAnhang in der
Ergänzung ) aufgenommen. Es wurde eine elektronische Einwilligungserklärung eingeholt, und die Studie wurde vom institutionellen Überprüfungsausschuss für menschliche Teilnehmer der University of Washington genehmigt. Diese Studie folgte der Stärkung der Berichterstattung über Beobachtungsstudien in der Epidemiologie (
STROBE) Berichterstattungsrichtlinie. COVID-19-Symptomdaten wurden zum Zeitpunkt der akuten Erkrankung erhoben oder retrospektiv bei einem 30-tägigen Aufnahmebesuch erfasst. Zwischen August und November 2020 wurden insgesamt 234 Teilnehmer mit COVID-19 kontaktiert, um einen einzigen Follow-up-Fragebogen zwischen 3 und 9 Monaten nach Krankheitsbeginn auszufüllen. Wir haben für diese deskriptive Analyse aufgrund der geringen Anzahl in jeder Untergruppe keine statistischen Tests durchgeführt. Die Datenanalyse wurde in R Version 4.0.2 (R Project for Statistical Computing) durchgeführt.
Ergebnisse
A total of 177 of 234 participants (75.6%; mean [range] age, 48.0 [18-94] years; 101 [57.1%] women) with COVID-19 completed the survey. Overall, 11 (6.2%) were asymptomatic, 150 (84.7%) were outpatients with mild illness, and 16 (9.0%) had moderate or severe disease requiring hospitalization (
Table). Hypertension was the most common comorbidity (23 [13.0%]). The follow-up survey was completed a median (range) of 169 (31-300) days after illness onset among participants with COVID-19 (
Figure, A) and 87 (71-144) days after enrollment among 21 patients in the control group. Among participants with COVID-19, persistent symptoms were reported by 17 of 64 patients (26.6%) aged 18 to 39 years, 25 of 83 patients (30.1%) aged 40 to 64 years, and 13 of 30 patients (43.3%) aged 65 years and older. Overall, 49 of 150 outpatients (32.7%), 5 of 16 hospitalized patients (31.3%), and 1 of 21 healthy participants (4.8%) in the control group reported at least 1 persistent symptom. Of 31 patients with hypertension or diabetes, 11 (35.5%) experienced ongoing symptoms.
The most common persistent symptoms were fatigue (24 of 177 patients [13.6%]) and loss of sense of smell or taste (24 patients [13.6%]) (
Figure, B). Overall, 23 patients (13.0%) reported other symptoms, including brain fog (4 [2.3%]). A total of 51 outpatients and hospitalized patients (30.7%) reported worse HRQoL compared with baseline vs 4 healthy participants and asymptomatic patients (12.5%); 14 patients (7.9%) reported negative impacts on at least 1 activity of daily living (ADL), the most common being household chores.
Discussion
In this cohort of individuals with COVID-19 who were followed up for as long as 9 months after illness, approximately 30% reported persistent symptoms. A unique aspect of our cohort is the high proportion of outpatients with mild disease. Persistent symptoms were reported by one-third of outpatients in our study, consistent with a previously reported study,
4 in which 36% of outpatients had not returned to baseline health by 14 to 21 days following infection. However, this has not been previously described 9 months after infection.
Consistent with existing literature, fatigue was the most commonly reported symptom.
2-
4 This occurred in 14% of individuals in this study, lower than the 53% to 71%
2-
4 reported in cohorts of hospitalized patients, likely reflecting the lower acuity of illness in our cohort. Furthermore, impairment in HRQoL has previously been reported among hospitalized patients who have recovered from COVID-19; we found 29% of outpatients reported worsened HRQoL.
5
Notably, 14 participants, including 9 nonhospitalized individuals, reported negative impacts on ADLs after infection. With 57.8 million cases worldwide, even a small incidence of long-term debility could have enormous health and economic consequences.
6
Study limitations include a small sample size, single study location, potential bias from self-reported symptoms during illness episode, and loss to follow-up of 57 participants. To our knowledge, this study presents the longest follow-up symptom assessment after COVID-19 infection. Our research indicates that the health consequences of COVID-19 extend far beyond acute infection, even among those who experience mild illness. Comprehensive long-term investigation will be necessary to fully understand the impact of this evolving viral pathogen.
Back to top